Ankle Pain: Symptoms, Causes, Treatment and When to See a Physio
Ankle pain is one of the most frequent injuries seen by physiotherapists — affecting office workers, runners, and athletes alike. Whether it’s pain after a sprain, stiffness when walking, or recurring discomfort during exercise, understanding the cause is the first step towards full recovery and confidence in movement.

What is Ankle Pain?
Ankle pain refers to discomfort, swelling, or stiffness around the ankle joint. It often results from a sprain, overuse, or reduced control through the foot and leg muscles. Sometimes, pain can persist after an old injury that hasn’t completely healed or been retrained properly. An ankle pain physio will assess your joint stability, strength, and alignment to identify exactly which structures are involved and tailor a plan to restore balance, stability, and pain‑free movement.
Main Types of Ankle Pain
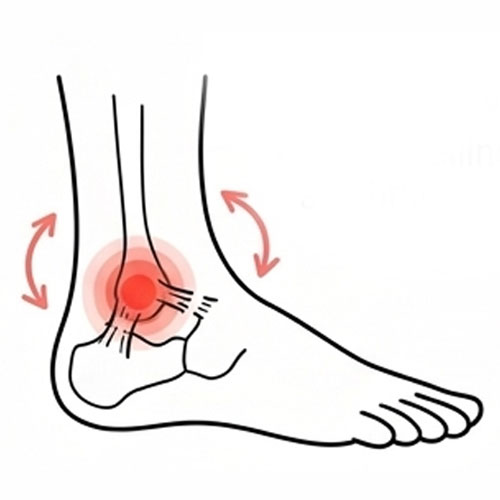
Ankle Sprain (Ligament Injury)
Common in active adults or older individuals, felt deep in the front of the hip.
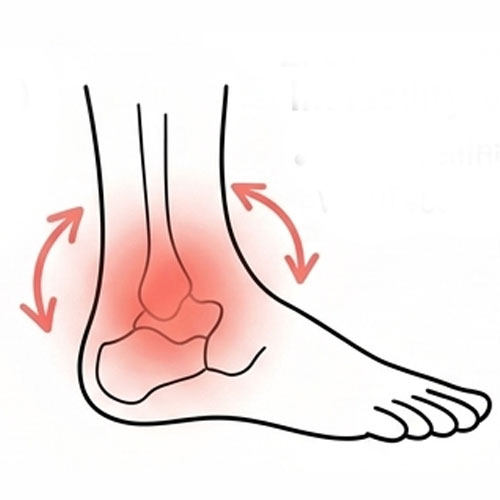
Chronic Ankle Instability
Pain and tenderness
on the outside of the hip, often worse when lying on the affected side.
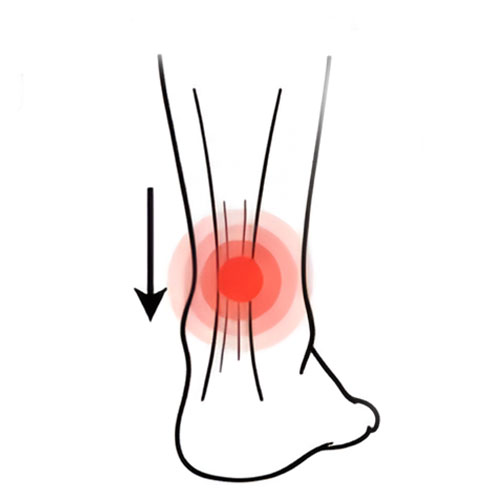
Achilles Tendonitis or Tendinopathy
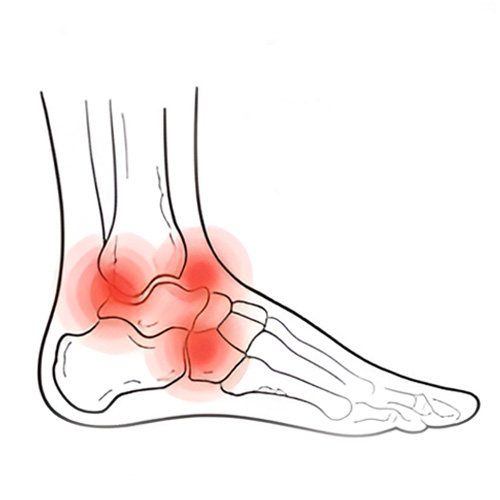
Posterior Tibial Tendon Dysfunction (Flat Foot)
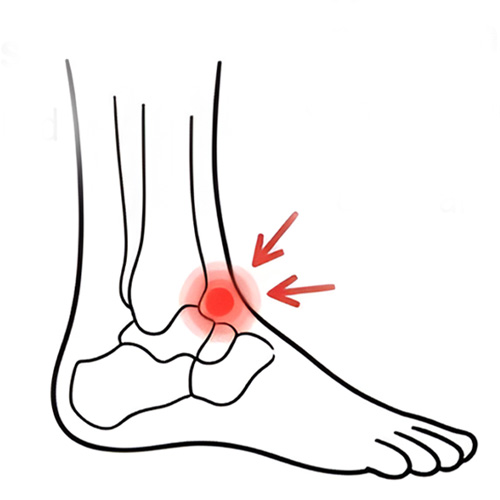
Ankle Impingement

Arthritis or Degenerative Changes
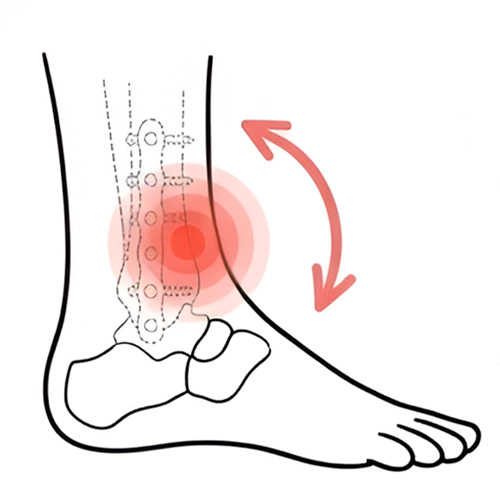
Post‑Fracture or Post‑Surgical Pain
Common Causes and Contributing Factors
- Previous ankle sprain or injury leading to instability
- Overuse from running, jumping, or long‑distance walking
- Weak calf, hip, or foot muscles
- Poor footwear or sudden change in activity
- Flat feet or high arches altering ankle mechanics
- Limited calf flexibility or joint stiffness
- Poor balance and proprioception
For some, an exact cause isn’t always found; instead, back pain can result from the combined load of lifestyle, posture, and movement habits.
Symptoms and What They Mean
- Sharp or aching pain around the ankle joint
- Swelling, redness, or bruising after injury
- Stiffness or reduced motion, especially in the morning
- Pain walking on uneven surfaces or stairs
- Clicking, catching, or instability (“giving way”)
- Tightness in the calf or tendon area
A skilled ankle pain physiotherapist can identify patterns, test joint integrity, and rule out serious conditions before creating a rehabilitation programme tailored to your lifestyle and goals.
How Long Does Ankle Pain Last?
Acute ankle pain (under 6 weeks): Sprains or new overload injuries often settle quickly with structured care.
Persistent or chronic ankle pain (12+ weeks): Benefits most from comprehensive rehab that rebuilds strength, control, and confidence.
Sub‑acute pain (6–12 weeks): May require ongoing strengthening, stability work, and movement retraining.
When Ankle Pain Needs Urgent Attention (Red Flags)
- Sudden severe swelling or deformity after injury
- Inability to bear weight or walk more than a few steps
- Persistent numbness, tingling, or coldness in the foot
- Signs of infection (redness, warmth, fever)
- Unexplained night pain or rapid worsening of swelling
How Physiotherapists Diagnose Ankle Pain
During your first appointment, your ankle pain physio will:
- Take a detailed history of your injury, exercise routine, and footwear
- Assess joint range, swelling, and alignment in standing and walking
- Test muscle strength, balance, and stability
- Identify if pain stems from ligaments, tendons, or joint surfaces
- Perform specific tests to rule out fracture or severe ligament rupture
If needed, your physiotherapist can arrange imaging (X‑ray, MRI, or ultrasound) and coordinate with your GP or specialist for comprehensive care.
Physiotherapy Treatment for Ankle Pain
Depending on the diagnosis, treatment may include:
Hands‑On Physiotherapy
Exercise Therapy
Movement and Balance Retraining
Rehabilitation Programmes
How Physiotherapy Helps Long Term
- Restoring normal joint mobility and alignment
- Strengthening key stabilising muscles
- Strengthening key stabilising muscles
- Reducing swelling and stiffness
- Enhancing performance and preventing long‑term recurrence
When to See a Physio
You should see a physiotherapist if:
- Pain persists for more than a few days or repeatedly returns
- You struggle to walk, run, or balance normally
- Swelling or stiffness limits daily movement
- Pain wakes you at night or worsens with exercise
- Over‑the‑counter medication or rest isn’t helping
Take the Next Step Toward Recovery
At One Body, our physiotherapists specialise in ankle pain treatment — from ankle sprains and Achilles tendon injuries to post‑surgical rehabilitation. We combine advanced assessment, hands‑on treatment, and tailored exercise programmes to get you moving confidently again.

This page has been medically reviewed by Rebecca Bossick, Lead Clinical Physiotherapist, HCPC & CSP Registered.

