Back Pain: Symptoms, Causes and When to Get Help
Back pain is one of the most common muscle and joint problems, affecting people of all ages and activity levels. It can feel like a dull ache after sitting, sharp pain when bending, stiffness in the morning, or pain that travels into the buttock or leg. Understanding what may be driving your symptoms is the first step towards safer, more confident recovery.
Most episodes improve with the right advice, movement and self-management, but persistent, recurrent or worsening back pain is a sign that you may benefit from a professional physiotherapy assessment.
🛑 Important Notice: This content covers topics that may significantly impact your wellbeing. We recommend consulting a qualified healthcare professional before acting on this information, especially if your symptoms are severe, worsening, unusual, or affecting your bladder, bowel, balance, walking, strength or sensation.
Medically reviewed by Rebecca Bossick, Lead Clinical Physiotherapist, HCPC & CSP Registered.
Last reviewed: May 2026
Key Takeaways
- Most back pain is “non-specific”, meaning there is not always one single structure, scan finding or injury that fully explains the pain.
- Back pain often improves with movement, self-management and time, but it can become persistent if the underlying contributors are not addressed.
- Staying active and avoiding prolonged bed rest is usually more helpful than complete rest for most mechanical back pain.
- Red flag symptoms such as loss of bladder or bowel control, numbness around the groin or saddle area, or severe/progressive leg weakness require urgent medical attention.
- Physiotherapy may help when back pain is linked to movement, strength, mobility, nerve sensitivity, work demands, training load or recurring flare-ups.
- Pain does not always mean damage. Stress, poor sleep, prolonged sitting, reduced strength, fear of movement and nervous system sensitivity can all affect how intense back pain feels.
- If your back pain has not improved after four to six weeks, keeps returning, or is affecting work, sleep, training or day-to-day life, a physiotherapy assessment can help you understand the cause and plan your recovery.

What is Back Pain?
Back pain refers to discomfort or stiffness felt anywhere from the neck to the pelvis. It can range from mild muscle tightness to severe nerve irritation that radiates down the leg.
In many cases, back pain relates to irritation, strain or overload of muscles, joints, discs or nerves in the spine. However, pain is not always caused by one single structure. A proper assessment looks at your symptoms, movement, strength, lifestyle, work demands and activity levels to understand what may be contributing to the problem.
Clinicians usually classify back pain by the area affected. Cervical pain refers to the neck, thoracic pain refers to the mid-back, and lumbar pain refers to the lower back. Lower back pain is the most common because the lumbar spine takes a large amount of load during sitting, bending, lifting, walking, running and training.
Back pain is also classified by how long it has been present. Acute back pain is recent and short-term. Sub-acute back pain lasts longer and may need a more structured plan. Chronic or persistent back pain usually means symptoms have lasted for around three months or more. Understanding where you are in this timeline helps guide treatment, exercise selection and expectations for recovery.
A key point is that most back pain is not caused by one simple “fault” in the spine. In many cases, pain comes from a combination of irritated joints, muscles, discs, nerves, movement habits, reduced strength, lifestyle load and nervous system sensitivity. This is why a good assessment looks at your symptoms, movement, strength, work demands, training history, sleep, stress and previous injuries — not just one painful structure.
What Anatomy Is Involved in Back Pain?
Your spine is made up of vertebrae stacked on top of each other, with intervertebral discs between them acting as shock absorbers. Ligaments help hold the vertebrae together, while muscles and tendons provide movement, control and support.
The spinal cord runs through the spinal canal, with nerves exiting at different levels to supply the trunk, pelvis, legs and feet.
The lumbar spine, which is the lower part of your back, carries a high amount of load. This is why lower back pain is so common in people who sit for long periods, lift weights, play sport, commute, bend frequently or spend long working days at a desk.
Each lumbar disc has a tougher outer ring and a softer gel-like centre. When people talk about a “slipped disc”, they are usually referring to a disc bulge or herniation where the inner part of the disc pushes outwards and may irritate a nearby nerve. The term “slipped disc” can be misleading because the disc does not literally slip out of place.
Facet joints sit at the back of each spinal segment and help guide movement. The sacroiliac joints connect the base of the spine to the pelvis.
Muscles such as the erector spinae, multifidus, quadratus lumborum, glutes, hip flexors and deep abdominal muscles all influence how the lower back moves and tolerates load.
Pain can come from any of these structures, but in many cases it is not one isolated tissue causing the whole problem. Back pain often develops from a combination of load, stiffness, weakness, sensitivity, posture habits, training errors, work demands and recovery factors.
Main Types of Back Pain
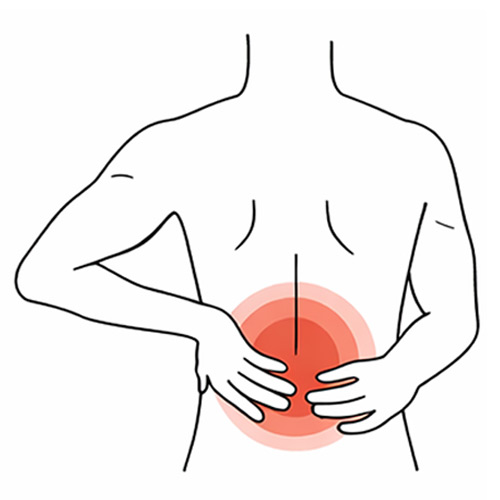
Lower Back Pain
(Lumbar Pain)
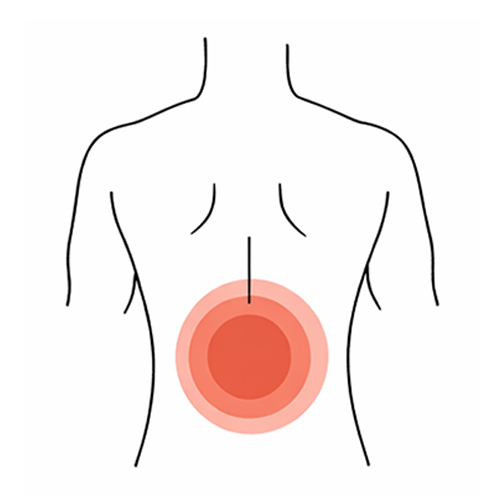
Mid‑Back Pain (Thoracic Pain)

Nerve Pain and Sciatica
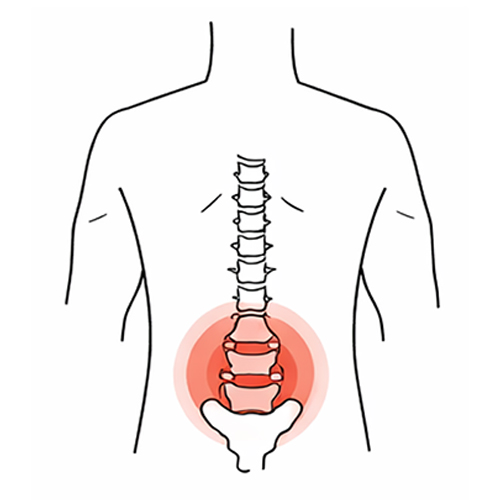
Disc‑Related Pain
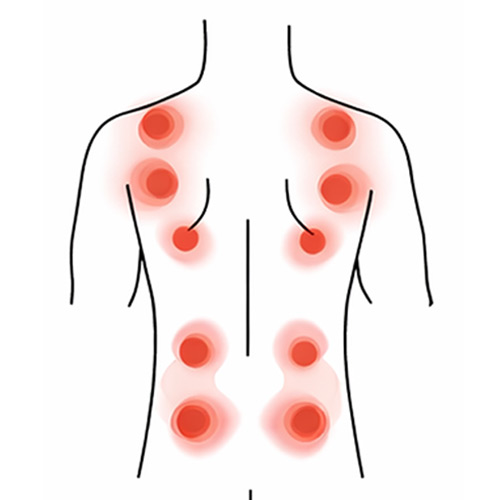
Arthritis and Age‑Related Changes
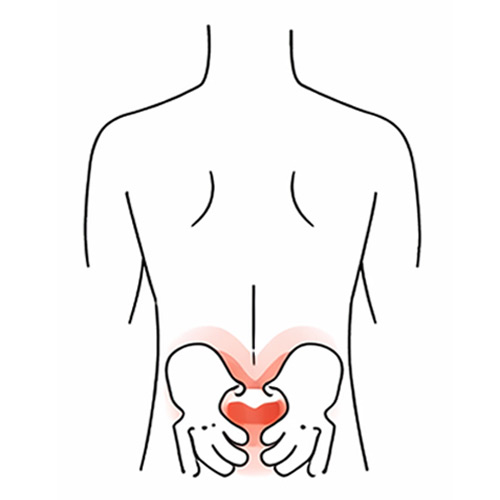
Sacroiliac Joint (SIJ) Pain
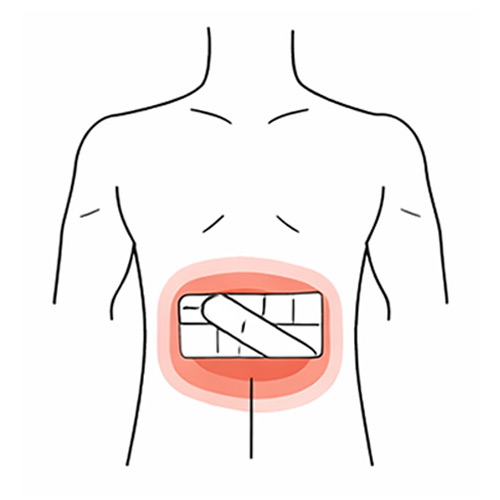
Post‑Operative or Post‑Injury Pain
Each type may need a slightly different approach, which is why assessment, symptom behaviour and individual goals matter.
Common Causes and Contributing Factors
Back pain can have several possible causes and contributors. In many cases, symptoms come from a combination of tissue sensitivity, movement habits, strength, lifestyle load, work demands and recovery factors rather than one single fault in the spine.
Muscle or Ligament Strain
Muscle or ligament strain can happen when the muscles and soft tissues around the spine are overloaded. This may follow lifting, twisting, sudden movement, sport, training or doing more activity than your body is currently prepared for.
Disc Irritation, Bulge or Herniation
A spinal disc can become irritated or bulge towards a nearby nerve root. This may contribute to lower back pain, leg pain, pins and needles or sciatica-like symptoms. However, disc changes can also appear on scans in people without pain, so imaging findings must always be matched with symptoms and clinical assessment.
Facet Joint Irritation
Facet joints are the small joints at the back of the spine. They can become stiff, sensitive or overloaded, especially with prolonged standing, repeated arching, extension-based movements or sudden increases in activity.
Degenerative or Age-Related Changes
Changes such as spinal osteoarthritis or disc degeneration are common with age. They do not always cause pain, but they may contribute to stiffness, sensitivity or reduced tolerance to certain positions and activities.
Spinal Stenosis
Spinal stenosis is narrowing around the spinal canal or nerve pathways. It is more common in older adults and may cause leg pain, heaviness, cramping or weakness when walking, often easing with sitting or bending forward.
Sacroiliac Joint Pain
Sacroiliac joint pain comes from the joint where the spine meets the pelvis. It can feel deep in one side of the lower back, buttock or pelvis and may be linked to pregnancy, altered loading, injury or changes in activity.
Post-Operative or Post-Injury Pain
Back pain can persist after trauma, surgery or a period of reduced activity. In these cases, graded rehabilitation may be needed to rebuild strength, confidence, mobility and movement tolerance.
Less Common but More Serious Causes
Less common but more serious causes of back pain can include fractures, infections, inflammatory conditions or, rarely, cancer. This is why a physiotherapist or healthcare professional should screen for red flags during assessment.
Why Does Back Pain Happen?
There is often a difference between the moment back pain starts and the real reason it developed. You might feel pain after bending down, lifting a bag, twisting awkwardly or getting out of bed, but the underlying issue may have been building for weeks or months.
For many London office workers, the pattern is familiar: long hours sitting at a desk, commuting, training inconsistently, sleeping poorly, then suddenly feeling back pain during a simple movement. Over time, reduced strength, stiff hips, limited thoracic mobility, deconditioning and repeated sitting can reduce your back’s tolerance to load.
Back pain can also be affected by stress. High stress can increase muscle tension, change breathing patterns, reduce sleep quality and make the nervous system more sensitive. This can make pain feel stronger even when there is no serious structural damage.
Poor sleep can also make pain harder to manage because it reduces recovery and increases sensitivity. Smoking, low physical activity, sudden spikes in training, obesity, poor recovery and long periods of sitting may also contribute.
This is why effective back pain management is rarely about one painful area alone. A good assessment looks at the whole picture: your spine, hips, strength, mobility, work setup, training load, recovery, sleep, stress and confidence with movement.
Symptoms and What They Mean
- A dull, persistent ache across the lower back, often worse after prolonged sitting or standing.
- Stiffness first thing in the morning that eases after gentle movement.
- Sharp or stabbing pain when bending, twisting, lifting or getting up from a chair.
- Pain that travels into one or both buttocks, or down the back of the leg, which may suggest nerve irritation or sciatica.
- Muscle spasm, tightness or guarding on one side of the spine.
- Difficulty straightening up after bending forward.
- Aching that worsens towards the end of a long working day, especially for desk-based professionals.
- Pins and needles, numbness or weakness in the leg or foot, which may suggest nerve involvement.
A clinical assessment can help identify pain patterns, screen for red flags and guide the right next step based on your symptoms, movement limitations and goals.
Some people also experience referred pain, where a back problem causes discomfort in a nearby area such as the hip, buttock, groin or thigh.
It is also important to separate morning stiffness from night pain. Morning stiffness is common and often improves after movement. Night pain that repeatedly wakes you, does not change with position, or is associated with feeling unwell, unexplained weight loss, fever or worsening neurological symptoms should be assessed medically.
What Does Back Pain Feel Like?
Back pain can feel very different from person to person. Some people describe it as a constant low-level ache, tightness or pressure across the lower back. Others feel sudden sharp pain, catching, locking, spasms, burning, or an electric shock sensation with certain movements.
If a nerve is irritated, pain may travel into the buttock, hamstring, calf or foot. This can feel like burning, shooting pain, pins and needles, numbness or weakness. This pattern is often associated with sciatica or nerve root irritation.
The way your pain behaves is often more useful than the exact word used to describe it. Mechanical back pain usually changes with movement or position. It may ease when walking but worsen with sitting, bending or lifting. Inflammatory-type pain may feel worse at rest, worse at night, or better with movement.
Pain is also influenced by the nervous system. Two people can have similar scan findings but completely different levels of pain. Stress, poor sleep, previous pain experiences, fear of movement and worry about the back can all increase sensitivity. This does not mean the pain is “in your head”; it means pain is produced by the body and nervous system together.
A useful step before seeing a physiotherapist is to notice what makes your pain better, what makes it worse, whether it travels, whether it changes during the day, and whether it affects sleep, work, training or walking. This helps your physiotherapist understand the likely drivers of your pain.
How Long Does Back Pain Last?
Back pain is often grouped by how long symptoms have been present:
- Acute back pain: symptoms lasting less than 6 weeks. These episodes often improve within days to weeks with the right advice, gentle movement and self-management.
- Sub-acute back pain: symptoms lasting 6–12 weeks. This may need a more structured rehabilitation plan.
- Chronic or persistent back pain: symptoms lasting 12 weeks or longer. This often benefits from a combined approach that includes education, graded exercise, strength work, lifestyle changes and confidence-building around movement.
Getting the right advice early can help you avoid unnecessary fear, prolonged rest and repeated flare-ups.
Most simple episodes of back pain improve within a few weeks, especially when you stay gently active and avoid prolonged bed rest.
Some cases settle quickly, while others take longer depending on the severity of symptoms, whether nerve pain is involved, your activity levels, your work demands and whether the same triggers keep repeating.
Back pain lasting beyond a few weeks does not automatically mean something serious is wrong, but it does suggest that your body may need a more structured recovery plan.
Symptoms that last beyond 12 weeks are more likely to need a combination of education, graded exercise, strength work, manual therapy where appropriate, lifestyle changes and confidence-building around movement.
Signs your back pain is improving include better movement, less morning stiffness, fewer flare-ups, improved walking tolerance, better sleep, reduced leg symptoms, and being able to return gradually to work, training or normal daily activities.
Signs your back pain may need further help include pain that is getting worse, pain travelling further down the leg, increasing numbness or weakness, repeated flare-ups, or pain that keeps stopping you from working, exercising or sleeping normally.
When Does Back Pain Need Urgent Medical Attention?
Most back pain is mechanical and improves with movement, self-management and time. However, some symptoms need urgent medical attention because they may suggest a more serious problem.
Call 999 or go to A&E if you have back pain with:
- Loss of bladder or bowel control
- Difficulty passing urine or new changes in bladder or bowel function
- Numbness, tingling or loss of sensation around the groin, genitals, inner thighs or saddle area
- Severe or rapidly worsening weakness in one or both legs
- Pain, tingling, weakness or numbness affecting both legs
- Back pain after significant trauma, such as a fall from height or road traffic accident
- Chest pain alongside back pain
Seek urgent GP advice or call 111 if you have back pain with:
- Fever, chills or feeling generally unwell
- Unexplained weight loss
- A history of cancer with new back pain
- Pain that is constant, does not change with position, or repeatedly wakes you at night
- Pain that is getting worse quickly
- Progressive numbness, pins and needles or weakness
A physiotherapist can assess mechanical back pain, screen for red flags and refer you onwards if medical investigation is needed. If you are unsure whether your symptoms are safe for physiotherapy, it is better to seek medical advice early rather than wait.
How Is Back Pain Diagnosed?
A back pain diagnosis usually starts with a detailed conversation about when the pain started, where you feel it, what makes it better or worse, whether symptoms travel into the legs, and whether there are any red flag signs that need medical review.
A physiotherapy assessment may include:
- A full history of your symptoms, lifestyle, work demands, training and previous injuries
- Screening questions for red flags and symptoms that may need medical review
- Observation of posture, walking and movement patterns
- Active range of motion testing, such as bending, twisting, extending and side-bending
- Strength testing of the hips, legs, trunk and core
- Neurological testing, including reflexes, sensation and muscle strength where nerve involvement is suspected
- Clinical tests for the discs, facet joints, sacroiliac joints and nerve roots where appropriate
- Functional testing based on your goals, such as squatting, hinging, lifting, sitting tolerance, running or sport-specific movement
If imaging (like an MRI or X‑ray) is required, your physiotherapist can communicate
findings to your GP or specialist as part of an integrated care approach.
Imaging such as MRI or X-ray is not routinely needed for most non-specific back pain. Scans can be useful when serious pathology is suspected, symptoms are not improving as expected, or the result would change the management plan.
Many people have disc bulges, degeneration or age-related changes on scans without any pain, so imaging should always be interpreted alongside your symptoms and physical assessment.
In most cases, a careful clinical assessment gives enough information to begin a safe and effective treatment plan.
How Is Back Pain Usually Treated?
Back pain treatment depends on the type, severity and duration of symptoms. For most people, the best approach is active rather than passive. This means understanding the pain, keeping moving where safe, improving strength and mobility, and gradually rebuilding confidence in normal activity.
Common treatment options include:
-
Self-management and education: Understanding your pain, staying active, pacing activities and knowing what to avoid during a flare-up.
-
Physiotherapy: Assessment, advice, hands-on treatment where appropriate, movement testing, exercise prescription, strength work and a clear recovery plan.
-
Exercise and rehabilitation: Structured exercises to improve strength, flexibility, control, endurance and load tolerance.
-
Manual therapy: Joint mobilisation, soft tissue treatment or massage-based techniques used alongside exercise and advice to help reduce pain and improve movement where appropriate.
-
Medication: Short-term anti-inflammatory medication may help some people, but it is not a long-term solution and may not be suitable for everyone. Paracetamol alone is not usually recommended for back pain.
-
Psychological approaches: Education, reassurance, confidence-building and cognitive behavioural approaches can help persistent pain, especially when fear, stress or avoidance are contributing.
-
Injections: In some specific cases, such as severe nerve-related leg pain, injections may be considered by a specialist.
-
Surgery: Surgery is only considered for specific structural problems where symptoms, examination findings and imaging all match, and where conservative care has not helped.
For most back pain, prolonged bed rest is not helpful. Gentle activity, graded exercise and a structured plan usually produce better long-term results.
Where Does Physiotherapy Fit Into Back Pain Care?
Physiotherapy can be helpful when back pain is affecting movement, work, sleep, training or day-to-day life, or when symptoms keep returning. The aim is not only to reduce pain in the short term, but to understand what is contributing to the problem and build a plan that helps you move with more confidence.
In your first appointment, your physiotherapist will ask about your pain history, work demands, training, sleep, stress, previous injuries and goals. They may then assess your movement, strength, joint mobility and nerve function where needed. From there, they can explain what is likely happening and outline a clear plan.
Treatment may include hands-on therapy, soft tissue techniques, movement advice, strength work, mobility exercises, graded exposure to painful movements and a progressive return to normal activity. At One Body LDN, sessions are designed to combine hands-on treatment with practical rehabilitation where clinically appropriate.
A good back pain plan should help you understand what is safe, what to avoid during a flare-up, how to rebuild strength, and how to reduce the chance of the same problem repeatedly coming back.
What Exercises and Rehab Help Back Pain?
Exercise is one of the most important long-term tools for managing and preventing back pain. The right exercises depend on your symptoms, stage of recovery, strength, confidence, lifestyle and goals.
In the early phase, gentle movement is usually best. This may include short walks, pelvic tilts, supported knee rolls, gentle mobility drills and comfortable changes of position throughout the day. The aim is not to force through pain, but to reduce stiffness and keep the back moving safely.
As symptoms settle, rehabilitation usually becomes more structured. This may include:
- Core control exercises such as dead bugs, bird-dogs and modified planks.
- Glute and hip strengthening such as bridges, clamshells, step-ups and squats.
- Thoracic mobility work such as open books, seated rotations and thread-the-needle movements.
- Hip flexor and hamstring mobility to reduce stiffness linked to prolonged sitting.
- Gradual loading through hinges, squats, carries and lifting patterns.
- Return-to-sport or return-to-gym progressions for runners, lifters and athletes.
For persistent back pain, the key is graded exposure. This means starting below your current tolerance and gradually building up. Over time, this helps reduce sensitivity, rebuild strength and improve confidence with the movements you may have been avoiding.
Lifestyle habits matter too. If you sit at a desk, take regular movement breaks. If you train, avoid sudden jumps in volume or intensity. If sleep is poor, recovery may be slower. If stress is high, pain may feel more intense. A complete rehab plan should consider all of these factors.
How Can You Reduce the Risk of Back Pain Coming Back?
Long-term back pain recovery is about increasing capacity. Capacity means your back can tolerate more sitting, walking, lifting, running, training, stress and day-to-day activity without repeatedly flaring up.
Reducing the risk of recurring back pain usually involves improving:
-
Strength: building the muscles that support your spine, hips and pelvis
-
Mobility: restoring movement through the spine, hips and surrounding joints
-
Load tolerance: gradually increasing how much your back can handle
-
Confidence: reducing fear of movement and understanding what is safe
-
Movement control: improving how you bend, lift, twist, sit, stand and train
-
Recovery habits: addressing sleep, stress, pacing, desk setup and training errors
-
Early warning signs: knowing how to respond before a small flare-up becomes a major setback
The goal is not just to feel better for a few days. It is to understand your back, return to normal activity, and reduce the risk of the same problem repeatedly coming back.
When Should You Get Help for Back Pain?
You should consider getting professional help for back pain if:
- Your pain has not improved after four to six weeks of self-management
- Your pain keeps returning or is becoming more frequent
- Pain is affecting your work, sleep, training or daily life
- You have pain travelling into the buttock, leg or foot
- You have pins and needles, numbness or weakness
- You are unsure whether it is safe to exercise, run, lift or return to sport
- You have lost confidence in your back
- You keep relying on painkillers without understanding what is driving the problem
- You want a clear assessment, treatment plan and exercises tailored to your situation
You should seek urgent medical help instead if you have red flag symptoms such as changes in bladder or bowel control, numbness around the saddle area, severe or progressive leg weakness, fever, unexplained weight loss, chest pain, or back pain after major trauma.
Many people wait too long before getting help. Early assessment can help stop a short-term episode becoming a long-term pattern, especially if you are avoiding movement, losing strength, sleeping poorly or repeatedly flaring up with work or training.
Back Pain FAQs
What does back pain feel like?
What does back pain feel like?
Back pain can feel like a dull ache, sharp stab, tight band, spasm, burning sensation or catching pain with movement. If a nerve is involved, you may also feel shooting pain, pins and needles, numbness or weakness travelling into the buttock, leg or foot. The character of the pain can give clues, but the most important factor is how the pain behaves and how it affects your daily life.
What usually causes back pain?
What usually causes back pain?
Back pain can be linked to muscle or ligament strain, joint irritation, disc irritation, nerve sensitivity, reduced strength, prolonged sitting, sudden increases in activity, stress, poor sleep or previous injury. In many cases, back pain is caused by a combination of factors rather than one single structure.
Can back pain go away on its own?
Can back pain go away on its own?
Yes, many episodes of back pain improve with time, movement and self-management. However, if pain is not improving after a few weeks, keeps returning, travels into the leg, or affects work, sleep or training, a physiotherapy assessment can help identify the contributing factors and reduce the risk of it becoming persistent.
When should I worry about back pain?
When should I worry about back pain?
You should seek urgent medical help if back pain is linked with loss of bladder or bowel control, numbness around the groin or saddle area, severe or worsening leg weakness, pain or numbness in both legs, fever, unexplained weight loss, chest pain, or a serious accident. You should also seek help if pain is worsening, not improving, or significantly affecting your normal life.
Can physiotherapy help back pain?
Can physiotherapy help back pain?
Physiotherapy can help many types of back pain by assessing movement, strength, mobility, nerve function and daily triggers. Treatment may include advice, hands-on therapy where appropriate, movement retraining, strengthening exercises, mobility work and a progressive return-to-activity plan.
What are the usual treatment options for back pain?
What are the usual treatment options for back pain?
Treatment depends on the cause, severity and duration of symptoms. For many people, the most effective approach combines education, staying active, physiotherapy, graded exercise, lifestyle changes and hands-on treatment where appropriate. Medication, injections or surgery may be considered in specific cases, but they are not usually the first step for most mechanical back pain.
What should I read next if I have back pain?
What should I read next if I have back pain?
If you want practical advice, read our guides on back pain at work, back pain when running, back pain when lifting weights and back pain exercises. If you are looking for private treatment, visit our Back Pain Treatment in London page.
Need Help With Ongoing Back Pain?
If your back pain is not improving, keeps returning, or is affecting work, sleep, training or daily life, One Body LDN provides private back pain physiotherapy across London. Our physiotherapists combine assessment, hands-on treatment and tailored rehab plans where clinically appropriate.
References
- National Institute for Health and Care Excellence (NICE). Low back pain and sciatica in over 16s: assessment and management (NG59).
- NHS. Back pain overview.
- Hartvigsen J, Hancock MJ, Kongsted A, et al. What low back pain is and why we need to pay attention. The Lancet. 2018.
- Hayden JA, Ellis J, Ogilvie R, et al. Exercise therapy for chronic low back pain. Cochrane Database of Systematic Reviews. 2021.
- Brinjikji W, Luetmer PH, Comstock B, et al. Systematic literature review of imaging features of spinal degeneration in asymptomatic populations. American Journal of Neuroradiology. 2015.
- Chartered Society of Physiotherapy. Low back pain.

This page has been medically reviewed by Rebecca Bossick, Lead Clinical Physiotherapist, HCPC & CSP Registered.

